Spinal muscular atrophy (SMA) is a genetic disorder characterized by the loss of motor neurons in the spinal cord and the part of the brain that connects to the spinal cord. The loss of these specialized nerve cells results in muscle weakness and wasting (also known as atrophy) and affects the control of muscle movement. There are many SMA types, many of them appearing during infancy and early childhood.
The progressive muscle weakness and wasting can cause individuals with spinal muscular atrophy to lose the ability to walk and position themselves, resulting in the need for an electric wheelchair. There are complex rehab kids power wheelchairs that can be customized to meet your child’s needs. Features include specialized seating, positioning and electronics.
Kids Power Wheelchairs and Spinal Muscular Atrophy

The customizable Edge 3 Stretto® kids wheelchair is available with optional iLevel® power adjustable seat height, allowing kids to elevate up to 12 inches while driving at 3.5 mph. iLevel’s Extra Stability Technology® enhances safety for completing Mobility Related Activities of Daily Living (MRADLs) such as transferring, toileting, grooming and cooking. In addition to its customizable features, the Edge 3 Stretto wheelchair for kids also comes with LED front and rear fender lights. This allows your son or daughter to see and be safely seen while crossing streets or parking lots.
Kids Power Wheelchair Drive Control Options

Your child may benefit from expandable electronics like the Q-Logic 3 Advanced Drive Controls. These controls are customizable and expandable. Q-Logic 3 gives your child the independence of driving their electric wheelchair with a joystick. Standard with Bluetooth®, Q-Logic 3 also allows your child to operate his or her smart phone or tablet using the Q-Logic 3 screen.
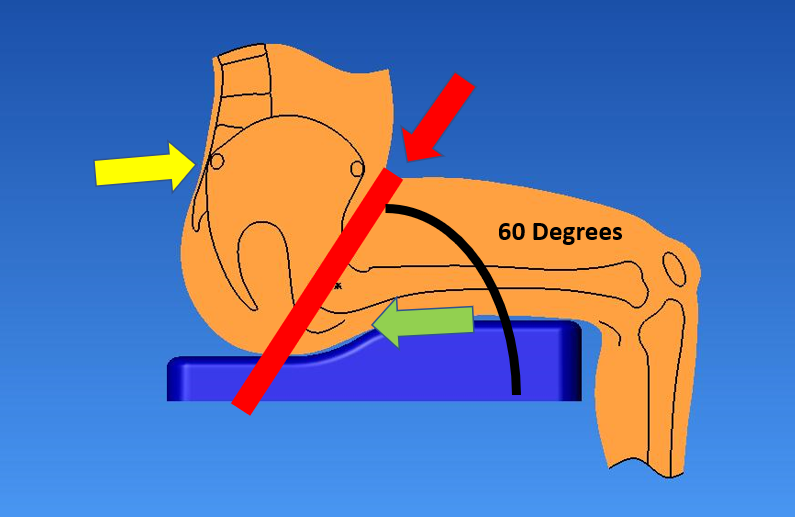
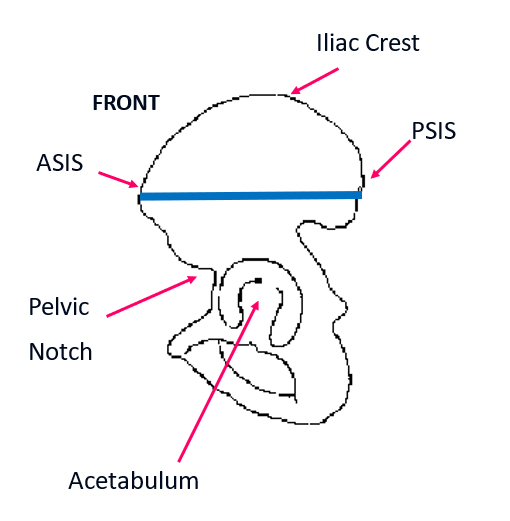
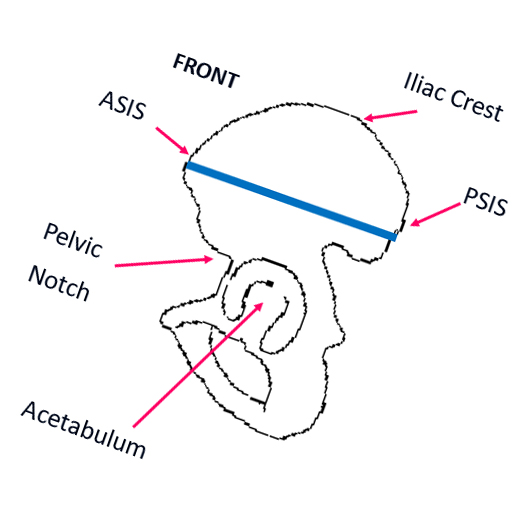
Wheelchair Positioning for a Kids Wheelchair
As their condition progresses, a child with spinal muscular atrophy may need power positioning on his or her electric wheelchair. This can assist with postural realignment, pressure relief and function. TRU-Balance® 3 Power Positioning Systems on electric child wheelchairs are highly adjustable and offer many medical benefits, including increased sitting tolerance, pressure relief, positioning for improved breathing and function and independent repositioning. Power tilt, power recline, iLevel, power articulating leg rests and power articulating foot platform are available options on TRU-Balance® 3.
Where to Buy a Kids Wheelchair
If you are looking to purchase a wheelchair for kids, you can visit an authorized Quantum provider. They can evaluate your child’s needs and determine if the Stretto is right for your child. Learn more on where to buy a wheelchair for kids.